Cancer treatment outcomes often depend on an overlooked biomarker — albumin.
During cancer treatment, many patients may receive the same therapy yet experience markedly different responses and levels of tolerance.
Research suggests that these differences are not solely related to the tumor itself, but are also closely linked to the patient’s overall physiological condition. One key indicator is albumin (Human Serum Albumin, HSA).
Multiple studies have shown that low albumin levels are significantly associated with higher rates of treatment interruption, increased risk of complications, and poorer overall prognosis in cancer patients (McMillan, 2001; Gupta & Lis, 2010).
Free cancer support
What is Albumin, and Why Is It Important in Cancer?
Albumin is the most abundant protein in human blood, accounting for about 50–60% of total plasma protein. It plays several essential physiological roles, including:
- Maintaining oncotic (colloid osmotic) pressure within blood vessels
- Transporting drugs, fatty acids, hormones, and vitamins
- Providing antioxidant and detoxification functions
- Supporting immune regulation and tissue repair
Research indicates that albumin is not just a nutritional protein, but also a natural transport and regulatory platform in the body. It plays a key role in drug distribution, metabolic balance, and immune responses (Fanali et al., 2012).
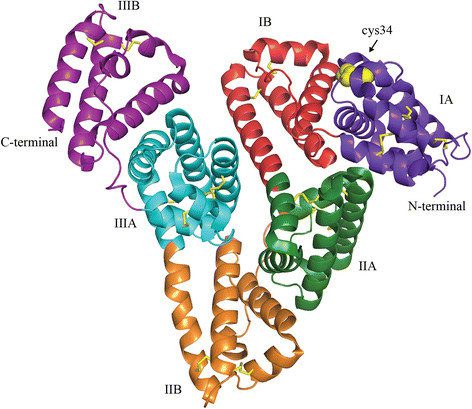
Common Issue of Low Albumin in Cancer Patients
Cancer-related chronic inflammation, metabolic changes, reduced appetite, and treatment side effects can all contribute to decreased albumin synthesis and increased breakdown.
Studies suggest that low albumin levels reflect not only inadequate nutritional intake, but are also closely associated with systemic metabolic imbalance and chronic inflammatory states (Levitt & Levitt, 2016).

Five Supportive Roles of Intravenous Albumin Therapy
1. Maintains Oncotic Pressure and Reduces Edema and Ascites
Albumin is the primary determinant of oncotic (colloid osmotic) pressure within blood vessels. When albumin levels are low, fluid can leak from the bloodstream into surrounding tissues, leading to edema and ascites, which may affect circulatory stability and increase physiological burden. Studies suggest that intravenous albumin may help restore intravascular fluid balance and support circulatory stability (Levitt & Levitt, 2016; Vincent et al., 2003).
2. Acts as a Natural Carrier to Enhance Drug and Nutrient Transport
Albumin can bind to various lipophilic drugs and endogenous molecules, prolonging their circulation time and improving bioavailability. Research indicates that albumin serves as an important platform for modern drug delivery systems and half-life extension strategies (Fanali et al., 2012; Sleep et al., 2013).
3. Provides Antioxidant and Anti-inflammatory Support
Albumin has significant antioxidant properties, helping to neutralize free radicals and bind potentially harmful metabolites. It may play a buffering and regulatory role in chronic inflammatory states. Studies highlight albumin’s role in reducing oxidative stress and modulating inflammatory responses (Roche et al., 2008; Ghuman et al., 2020).
4. May Support Drug Delivery to Tumors and Reduce Toxicity
Tumor blood vessels are often highly permeable, allowing albumin to accumulate more readily in tumor tissues (known as the enhanced permeability and retention, or EPR, effect). In addition, some cancer cells may actively take up albumin as a source of energy and amino acids. This characteristic underpins the development of albumin-bound anticancer therapies. A well-known clinical example is albumin-bound paclitaxel (nab-paclitaxel, Abraxane). Phase III clinical studies have shown improved tumor response rates and reduced solvent-related toxicity in breast cancer patients (Gradishar et al., 2005).
5. Supports Immune Function and Tissue Repair
Low albumin levels have been associated with impaired immune function, delayed wound healing, and increased risk of infection. Supplementation through intravenous albumin may help improve protein availability, supporting immune responses and tissue repair processes (McMillan, 2001; Don & Kaysen, 2004).
The Role of Intravenous Albumin Therapy
Based on current evidence, intravenous albumin therapy is not an anticancer treatment, but rather a supportive care strategy. Its core aims are to:
- Stabilize the body’s internal physiological environment
- Support drug function and treatment tolerance
- Help patients better complete their prescribed treatment plan

Conclusion
In cancer treatment, the body’s readiness to tolerate therapy is often just as important as the treatment itself.
Intravenous albumin therapy provides a supportive foundation that may help treatment proceed more smoothly, rather than replacing any anticancer therapies.
If you would like to learn more, feel free to contact our care team
for more detailed information and guidance.

Want to know more about Intravenous Albumin Therapy?


