Personalised Cancer Plan
Make treatment decisions with greater confidence
Precision insights that complement standard oncology care to guide next-step planning and ongoing monitoring.
=Why do I need this test if I already have a diagnosis?
What is Personalised Cancer Care
A Personalised Cancer Plan combines standard mainstream treatments with precision medicine to guide intelligent and individualized treatments.
In a published study, researchers observed encouraging results for patients receiving precision oncology compared with standard care.
In a published study comparing matched vs non-matched approaches:1,2
- Median overall survival: 11.4 vs 8.6 months
- Time without progression: 4.0 vs 2.8 months
- Tumor response observed in 27% vs 5% of patients
- Disease control reported in 70% vs 27%
Matching treatment to a patient’s cancer profile may be associated with more favorable outcomes.
Median overall survival (Months)1,2
m
m
therapy
therapy
Median progression-free survival (months)1,2
m
m
therapy
therapy
A Personalised Cancer Plan
(CTCs) analysis
(ctDNA) profiling
Key findings from a published study:1,2










In patients with advanced cancer, around 4 out of 10 in a matched treatment group experienced tumor response or disease stabilization for a period of time.
(Comparing matched vs non-matched treatment approaches)
Treatment Choice May Influence Outcomes1,2
Higher tumor response was observed in patients receiving matched approaches compared to non-matched approaches in a published study.
1. Results observed in a published study. Individual outcomes may vary.
2. Source: Tsimberidou et al., 2014, Journal of Clinical Oncology (MD Anderson IMPACT study, n=1,144). Study conducted in advanced cancer patients comparing matched and non-matched approaches.
Genetic testing of tumors may help guide
more personalized treatment decisions1,2










1. Results observed in a published study. Individual outcomes may vary.
2. Source: Rosell et al., 2013; Lindeman et al., 2018.
Studies on molecular profiling in lung cancer, including the identification of actionable mutations in a subset of patients and its role in supporting treatment planning. Findings may vary depending on patient and testing approach.
Contact our professional team now
Why Liquid Biopsy Testing
May Be Worth Considering
A personalised cancer plan may help guide more informed treatment choices by identifying drug-response insights before major treatment costs are incurred.
| Cost comparison | Estimated cost |
|---|---|
| Liquid biopsy (CTC test) | US$1,000–US$3,000 |
| One ineffective chemotherapy cycle | US$8,000–US$50,000+ |
| 6-month chemotherapy course | US$27,000–US$150,000+ |
1. Cost figures shown are illustrative ranges and may vary by country, treatment regimen, provider, and individual case.
2. Liquid biopsy may provide additional guidance for treatment decision-making, but does not guarantee outcomes or replace clinical judgment.
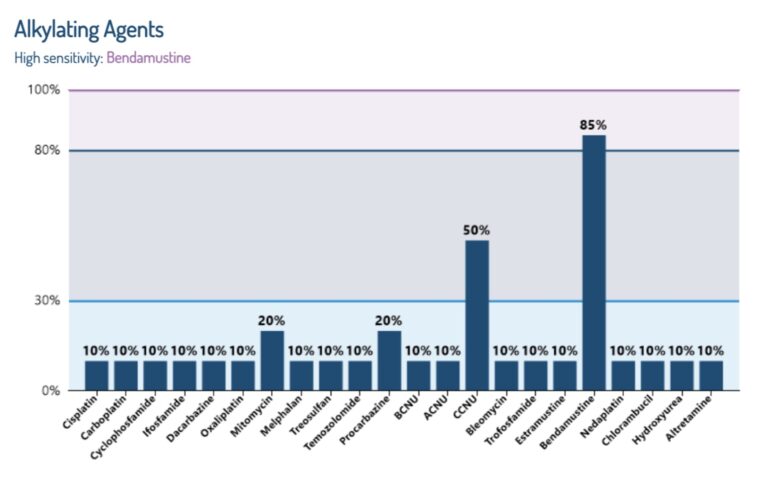
Example of a drug sensitivity report
This image shows an example of a laboratory drug sensitivity analysis, which evaluates how cancer cells may respond to different anticancer treatments.
The findings may help doctors identify therapies that could be more effective and avoid treatments that are less likely to work, together with other clinical information.
Understanding Your Precision Report
A precision report adds biological insight to standard clinical findings. It helps your doctor interpret risk, identify relevant options, and monitor changes over time — to support treatment decision-making.
What the report helps clarify
Structured insights can support your oncology team to plan with more confidence.
- ✓Actionable signals: findings that may support treatment selection or sequencing.
- ✓Monitoring clues: supports tracking response and detecting change earlier.
- ✓Risk context: helps interpret what “stable” or “progressing” may mean biologically.
How it complements standard care
| Area | Standard | With precision support |
|---|---|---|
| Decision basis | Clinical + imaging | Clinical + imaging + biological signals |
| Monitoring | Periodic scans | Scans + additional biological tracking |
| Adjustment | Often after visible change | May support earlier, informed adjustment |
| Goal | Follow evidence-based standards | Personalise choices using individual biology |
How it fits into your care journey
Speak to our team to learn what your report may indicate and how it can support treatment planning.
It works alongside standard cancer care to support more informed discussions with your healthcare team.
Response Rates in a published Study1,2
In recurrent ovarian cancer, biomarker-guided treatment was associated with differences in response rates in a published study
matched
therapy
(matched) therapy
Median Progression-Free Survival (months)1,2
Biomarker-guided treatment was associated with differences in progression-free intervals in a published study
matched
therapy
(matched) therapy
1. Results observed in a published study. Individual outcomes may vary.
2. Source: Herzog TJ et al., Gynecologic Oncology, 2010.
Study in recurrent ovarian cancer evaluating biomarker-guided (matched) therapy versus non-matched approaches.
In a precision medicine–guided approach, diagnosis is combined with biological assessment, allowing doctors to monitor both imaging and biological signals. This can support more informed treatment planning and adjustments over time.
Matched vs Non-Matched Therapy
Outcomes in a Published Study
Objective Response1,2
Rate (%)
Median Progression-1,2
Free Survival (months)
months
months
1. Results observed in a published study. Individual outcomes may vary.
2. Source: Herzog TJ et al., Gynecologic Oncology, 2010.
Study in recurrent ovarian cancer evaluating biomarker-guided (matched) therapy versus non-matched approaches.
Patients without Disease Progression at 2 Years (%)1,2
1. Results observed in a published study. Individual outcomes may vary.
2. Source: Pediatric MATCH trial (molecular profiling study). Evaluating outcomes with molecularly matched targeted therapy in pediatric patients.
- ✓ Detects genetic mutations
- ✓ Tracks tumour genetic evolution
- ✓ Useful for mutation monitoring over time
- ✕ Does not provide whole viable cancer cells
- ✓ Provides whole cancer cells for analysis
- ✓ Enables functional drug sensitivity testing
- ✓ Predicts survival across multiple solid tumours
- ✕ Not primarily used for detailed mutation tracking
References
Selected published studies and reviews relevant to precision medicine and biologically informed approaches in oncology.
| No. | Study Title / Citation | Year | Key Findings | Relevance |
|---|---|---|---|---|
| 1 |
Personalized medicine in a phase I clinical trials program: The MD Anderson Cancer Center initiative
Tsimberidou, A. M., Iskander, N. G., Hong, D. S., et al. (2014). Journal of Clinical Oncology, 32(8), 761–769.
|
2014 | Key findings Patients receiving matched therapies showed longer median overall survival (11.4 vs 8.6 months) and progression-free survival (4.0 vs 2.8 months) in this cohort. | Relevance Suggests that treatment matched to tumour biology may be associated with differences in outcomes in selected patients. |
| 2 |
Impact of precision medicine in diverse cancers: A meta-analysis of phase II clinical trials
Schwaederle, M., Zhao, M., Lee, J. J., et al. (2016). Journal of Clinical Oncology, 34(15), 1791–1799.
|
2016 | Key findings Higher response rates and longer progression-free survival were observed in patients treated with biomarker-matched therapies across pooled studies. | Relevance Indicates that biomarker-guided approaches may help inform treatment selection in certain settings. |
| 3 |
Pilot study using molecular profiling of patients’ tumors to find potential targets and select treatments for refractory cancers
Von Hoff, D. D., Stephenson, J. J., Rosen, P., et al. (2010). Journal of Clinical Oncology, 28(33), 4877–4883.
|
2010 | Key findings A proportion of patients experienced longer progression-free survival when treatment selection was guided by molecular profiling. | Relevance Suggests that profiling tumour characteristics may support more individualized treatment strategies. |
| 4 |
Cancer therapy directed by comprehensive genomic profiling: A single-center study
Wheler, J. J., Janku, F., Naing, A., et al. (2012). Cancer Research, 72(Suppl 8), 2776.
|
2012 | Key findings Some patients receiving matched therapies showed longer progression-free survival compared to prior treatments. | Relevance Highlights that integrating molecular data may provide additional insight for treatment planning. |
| 5 |
Clinical applications of circulating tumor cells and circulating tumor DNA as liquid biopsy
Alix-Panabières, C., & Pantel, K. (2016). Nature Reviews Clinical Oncology, 13(8), 479–491.
|
2016 | Key findings Liquid biopsy technologies provide information on tumour characteristics and disease monitoring across multiple cancer types. | Relevance Indicates that non-invasive testing approaches may offer additional biological information to support clinical decision-making. |
For educational purposes only. Findings are based on published studies. Outcomes may vary depending on tumour biology, stage, patient condition, and treatment context.


